The things I remember most about “Grammy” were the salmon sandwiches, Sunday dinner at the Golden Beaver and endless games of euchre. I remember going for long walks in the cemetery to visit Grandad, going to Stedman’s to buy a new model to put together and/or the daily trip to Ed’s In and Out to buy hockey cards. This is where my brother got his one and only Wayne Gretzky rookie card.
Last weekend was Mother’s Day so it was fitting to spend a moment to reflect on the “moms” in my life – my mother, my wife, my grandmothers, Oma Kaiser and Grammy Cargill. I knew her as Grammy but everyone else knew her by a different name: Florence Nightingale.
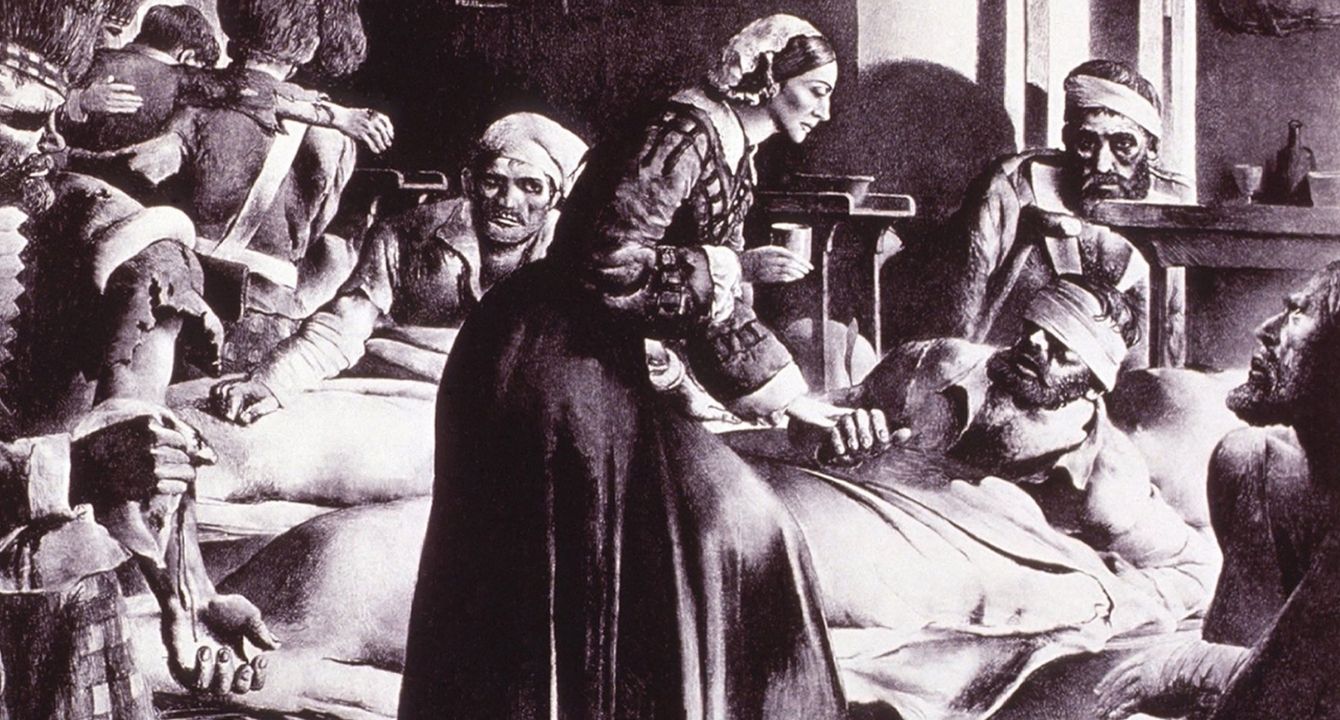
Ok, not THAT Florence Nightingale but still, she bore the name of the famous 19th-century nurse who founded modern nursing. Florence Nightingale came to prominence as a manager and trainer of nurses during the Crimean War, in which she organized care for wounded soldiers at Constantinople (Istanbul today). She gave nursing a favourable reputation and became an icon of Victorian culture, personified in art as The Lady with the Lamp making rounds of wounded soldiers at night.
Last week was National Hospice Palliative Care Week, so it comes as no surprise that it is followed by National Nurses Week. You can’t have one without the other.
In palliative care, there is what we call the Holy Trinity: doctors, nurses, social workers. Depending on the patient, each member of the interdisciplinary team brings their own unique skills and talents to bear. Dame Cicely Saunders, credited with starting the modern hospice and palliative care movement, was a nurse, but she was also a physician and a social worker. Saunders recognized that no one discipline could provide the holistic approach required for the seriously ill or terminal patient.
Let’s give nurses the floor for a moment, shall we?
“You ask me why I do not write something … I think one’s feelings waste themselves in words, they ought all to be distilled into actions and into actions which bring results.” ― Florence Nightingale
Nurses seem to be everywhere in palliative care. But to focus this discussion, I want to zoom in on some key areas: home care, hospice and administration.
Home care simply does not function without community nurses. 24/7/365, these “angels” care for seriously ill patients in their homes, providing hands-on care for our seniors as well as patients with cancer and other chronic illnesses. Like the mailman, they come no matter the season, no matter the weather. During the pandemic, they have continued unfailingly to support and care for patients in their homes.
“I am of certain convinced that the greatest heroes are those who do their duty in the daily grind of domestic affairs whilst the world whirls as a maddening dreidel.” ― Florence Nightingale
Nurse practitioners play a crucial role as well. Many are employed across Ontario specifically to provide palliative care, some in hospitals, many in the community and long-term care homes.
At the Hospice of Windsor, we have nurse educators. Their role, among many, is to provide real-time coaching and mentoring for community nurses and other health-care professionals. On a daily basis, it is amazing to hear them at work.
Sandy Buchman, past president of the Canadian Medical Association and Freeman Chair for Palliative Medicine at North York General Hospital, once called us at the Hospice of Windsor “the Valhalla of Palliative Care” in Ontario. Well, I certainly don’t see any Norse gods walking the campus but if that is the case, the nurse educators are the Valkyries.
Nurse educators are needed because the turnover in community nursing is high. Wages are low and most community nurses are drawn to higher paying jobs in hospitals or other settings. As such, the need for ongoing education is crucial. There is a never-ending battle to support and maintain the palliative competencies in our community nursing.
“What cruel mistakes are sometimes made by benevolent men and women in matters of business about which they can know nothing and think they know a great deal.” ― Florence Nightingale
Our hospice residences are staffed with RNs and RPNs who care for patients on a daily basis. Their role varies from day to day and is so much more than measuring vitals and administering medication. They wet the mouths of patients as they take their last breaths and continue to provide care while exhausted family members sleep on the pullout couch. Sometimes, they simply sit and are present so that no one dies alone.
“Live life when you have it. Life is a splendid gift ― there is nothing small about it.” ― Florence Nightingale
I enjoy making rounds at our hospice. When I meet a patient for the first time, I like to begin with an introduction: “Hello, my name is Dr. Cargill. I am here to take credit for the great work that the nurses are doing.”
This usually elicits a laugh or a chuckle. But it also serves to ground me and remind me that although I see these patients several times per week, our nursing staff sees these patients regularly and their insights and observations are invaluable in the care of our patients.
We also find great nurses in administration and supervisory roles. I have benefited from the experience of Allison Sherwood, Janet Elder, Fran Stanutz and Sheryl Johnston as palliative care coordinators at the Hospice of Windsor. They run our Palliative Medicine Program by, among many other things, managing new referrals and the schedule. Under their guidance, our program has maintained an average wait time of 3-5 days, with same day/next day visits available when needed. This is exceedingly rare in a medical system that routinely sees wait times of weeks to months, and in some cases years.
I have also been lucky to learn from individuals such as Janice Kaffer, CEO of Hotel Dieu Grace Health Care, and Monica Staley Liang, who stepped down as regional vice president of the Windsor Regional Cancer Centre and Renal Program a few months ago. Both have provided inspirational leadership and been unwavering champions of palliative care in Windsor-Essex and beyond.
“Let whoever is in charge keep this simple question in her head (not, how can I always do this right thing myself, but) how can I provide for this right thing to be always done?” ― Florence Nightingale
When I began my career as a palliative physician, the plan was for me to be mentored and trained by the incumbent physician. But like most plans, they change. She announced her retirement shortly after I arrived and left early due to burnout. As such, much of my early training in palliative care was not provided by physicians but by nurses. While I have learned much from my physician colleagues, I always remember that my early days were formed and shaped by countless days in a car, driving from one home to another, with a nurse at my side.
“So never lose an opportunity of urging a practical beginning, however small, for it is wonderful how often in such matters the mustard seed germinates and roots itself.” ― Florence Nightingale
Nurses are the glue of the health-care system. While we all have important roles to play in health care, as a physician, I can tell you that I simply could not do my job without them. So if you know a nurse, make sure to say “thanks” and let them know how much their work means to you and your family.
Back to Grammy, I never knew her as well as I would have liked. She died when I was young. But the memories I do have are fond ones. Because of her, I like coconut cream pies and cattails (typha), among other things. And yes, it was worth the drives to Acton.
I also know that Florence Pearl Nightingale, my Grammy, shared this in common with her namesake: “I attribute my success to this: never gave or took an excuse.” ― Florence Nightingale
#HappyNursesWeek2021


The comments section is closed.
Thank you Dr Cargill for all your support.
You’re welcome ;)
Please feel free to share stories below about the great nurses in your lives. #HappyNursesWeek